Monday to Friday, 7 AM – 7 PM CST.
Need help now? Fill out the form, and one of our experts will connect with you shortly.

Products and Services
ABA Practice Management and EMR Software. Your complete system to run and grow your practice
AI Driven Technology
%201.webp)
Artemis is transforming the ABA Therapy space with its innovative use of Salesforce Cloud, Automation, and AI based technology.
Our vision is to provide the first comprehensive, automated & AI-driven Practice Management & Billing software.
Technology Focused
At the heart of the Artemis ABA software is a focus on ensuring a simplified client intake process, automated eligibility check & authorization, optimized & AI-driven scheduling, automated claim scrubbing, real-time insurance claim status & analytics-based AR workflow.
It is critical for ABA Centers to get reimbursed by insurance in a timely and accurate manner. The goal is for an insurance claim to travel the shortest path from an ABA therapy session to an insurance payment with the use of the latest technologies.
Advanced Scheduling
%201.avif)
Simplified client scheduling. You make the appointment, and we will do the rest.
Our AI driven technology is helping practices spend less time managing their practice and more time caring for their clients.
We can imagine a practice where:
Care starts here. A professional practice runs on schedule.
With Artemis advanced scheduling you are connected to your practice in a meaningful way. Our scheduling system is designed to streamline your workflow using our AI driven technology to help you run and grow your practice.
Simplified booking, Artemis provides a comprehensive lens that simplifies your scheduling challenges.
Working with our customers to positively impact the industry by helping them grow their business while delivering the highest quality professional care.

Features
Comprehensive ABA
Practice Management

Our leading EMR software is designed to run and grow your practice. Get paid faster and spend less time managing your practice and more time with your patients.
Features
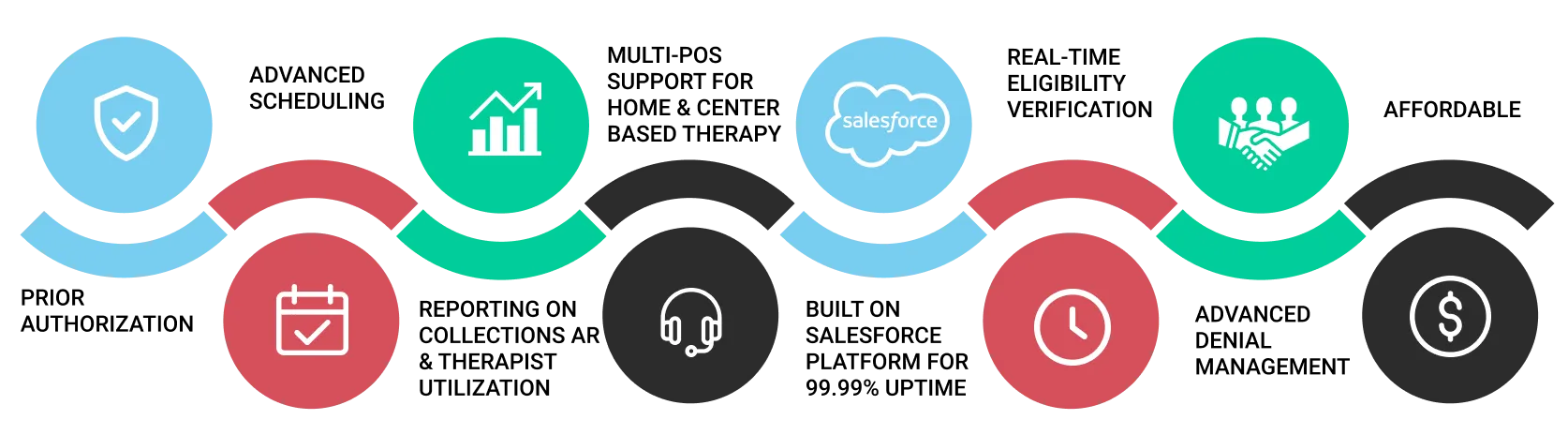
AI Powered Billing

We believe billing is one of the most important software features for a growing practice and it is at the foundation of our EMR. You might say Billing is in our DNA, well, maybe not but it is in our Cloud. Our goal at Artemis is for your claim to travel the shortest path from appointment to paid.
Features & Functions
Managed Billing Services
%201.webp)
Our clients enjoy custom strategies that are tailored to the unique revenue flow challenges of their practice or lab. Our dedicated team is ready to help you create a revenue growth action plan with automated, optimized processes.









%201.webp)


